The holidays are fast approaching and for many people, this part of the year is a fun time for celebrations and getting together with friends and family. For others however, the holidays can be sad and lonely, and a time of stress, anxiety, and depression. After the holidays, most people suffering with holiday blues bounce back, but for others, mood issues and depression are ongoing.
What is Depression?
According to the DSM-IV, a manual used to diagnose mental disorders, depression occurs when you have at least five of the following nine symptoms at the same time:
- a depressed mood during most of the day, particularly in the morning
- fatigue or loss of energy almost every day
- feelings of worthlessness or guilt almost every day
- impaired concentration, indecisiveness
- insomnia or hypersomnia (excessive sleeping) almost every day
- markedly diminished interest or pleasure in almost all activities nearly every day
- recurring thoughts of death or suicide (not just fearing death)
- a sense of restlessness — known as psychomotor agitation — or being slowed down – retardation
- significant weight loss or gain (a change of more than 5% of body weight in a month)
Benefits of Supplements for Depression
Although a much-overlooked therapy for depression, many nutritional supplements have been proven to be extremely beneficial without the side effects of anti-depressants. For those who would like to take a more natural approach to regulate their mood, there are many drug-free ways to improve the symptoms of depression. Here’s a look at 4 natural remedies for depression and their effectiveness based on scientific studies.
Rhodiola

Rhodiola
Thousands of years before antidepressants were developed, ancient civilizations were already experimenting with plants to treat emotional issues. Like Rhodiola rosea, for example, a perennial flowering plant native to the frigid mountains of Russia and Scandinavia, that has been used as a natural mood booster since the times of the Vikings.
Research shows that Rhodiola can have numerous benefits for the body and mind. In one 2015 study published in Phytomedicine, investigators compared the effects of Rhodiola with those of sertraline, an antidepressant known by the brand name Zoloft. For the study, 57 participants with depression were given a daily capsule of Rhodiola extract, medication, or placebo for a period of 12 weeks.
The results showed that both Rhodiola and Zoloft were effective at reducing symptoms of depression. The antidepressive effects of the prescription medication were higher, meaning that it was better at reducing depressive symptoms. However, the researchers noted that Rhodiola produced fewer side effects and was better tolerated by the volunteers, tilting the risk-benefit ratio in its favor.
In another study, participants given different doses of Rhodiola extract (340 mg or 680 mg) showed significant improvements in depression and insomnia scores compared to participants who only took a placebo. The results suggested that Rhodiola could be an effective supplement for treating depression even at lower doses.
5 HTP
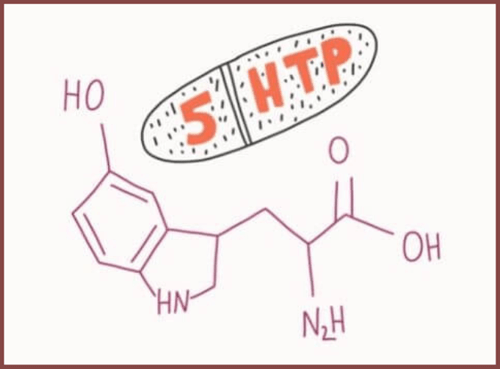
5 HTP
5-hydroxytryptophan, or 5 HTP for short, is a naturally occurring compound (meaning that your body produces it on its own) that could help improve the symptoms of depression. It plays many different roles in the body, but it’s mostly known for its potential to convert into serotonin, the so-called “happy” hormone.
Several studies have found that 5 HTP may be a good natural remedy for fighting depression. One clinical trial showed that 5 HTP was as effective as fluvoxamine, a selective serotonin reuptake inhibitor (SSRI), in treating mood disorders. This may be because 5 HTP could work similarly to SSRIs by increasing the amount of serotonin in the body.
Saffron Extract

A bottle of saffron extract
Saffron is the most expensive spice in the world, harvested from the stigmas of the Crocus sativus flower. A flower’s stigmas are the thread-like “whiskers” that extend from the bulb outwards to allow a female plant to receive pollen from a male plant. In the case of saffron, these threads are delicately collected by hand, one by one, hence the hefty price tag.
Among its many benefits, which include reducing symptoms of PMS, improving libido, and promoting weight loss, saffron is widely used as a natural antidepressant and mood booster. A review of studies published in Human Psychopharmacology concluded that saffron extract has similar antidepressant effects to prescription drugs. And a 2013 animal analysis found that saffron was capable of increasing dopamine levels in the brain without altering other neurotransmitters.
Methylfolate
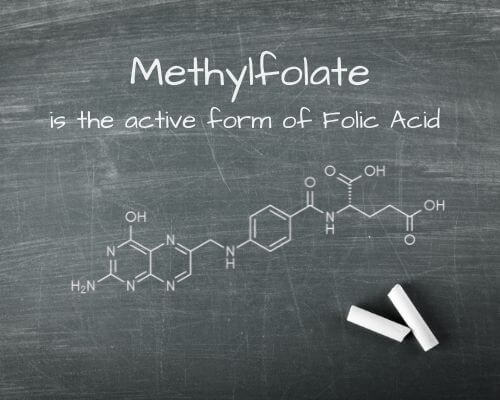
Methylfolate is the active form of folic acid
Methylfolate is a form of vitamin B known for its antidepressant properties. It may help improve mood by increasing levels of red blood cell folate, a deficiency that has been associated with major depressive disorder. The body also needs methylfolate to maintain adequate levels of serotonin, norepinephrine, and dopamine, three substances critical for normal brain function and behavior.
A Final Word About Nutritional Supplements for Depression
There’s no one-size-fits-all when it comes to treating depression – but never underestimate the power of nutrition. If you’re struggling with depression and looking for a more natural option, consider nutritional supplements proven effective in clinical studies, along with lifestyle changes to fit your individual needs.
For more information on natural alternatives for treating depression, download the white paper: Clinically Proven Natural Alternatives for Treating Depression.
Discover Resilient Mood – a nutritional supplement that helps balance mood and positive outlook