You’re at work staring at your computer screen when your forehead starts throbbing. You pop an over-the-counter pain med and brush it off as “just a bad headache.” When in fact, it could be a migraine.
Migraines affect over one billion people worldwide.1 While headaches are the textbook sign of migraine, they’re just one piece of the puzzle. So how can you tell if your headache is more than just a headache?
Read on to learn the difference between migraines and headaches and how to tell them apart.
What is a migraine?
For starters, it’s way more than just a bad headache. Migraine is a chronic neurological disorder that affects roughly 1 in 10 people.2
Throbbing head pain is the classic symptom of migraine. This usually occurs on one side of the head. However, some people may have pain on both sides.
Migraine attacks typically last between 4 to 72 hours.3 For some the pain is mild. For others, the pain can be severe enough to disrupt daily tasks – or even land them in the emergency room.
While migraine headaches can be intense, they’re not the only symptom. Migraine symptoms vary from to person and may include:4
- Neck pain
- Nausea or vomiting
- Sensitivity to light, sound, or smells
- Changes in mood
- Fatigue
- Trouble sleeping
- Visual disturbances
- Food cravings
- Trouble concentrating
What causes migraines?
It’s not entirely understood. But scientists say neuroinflammation may play a role. This can make the nerves overactive and trigger chemical changes in the brain. For people with migraine, this often looks like high levels of calcitonin gene-related peptide (CGRP) and low levels of serotonin.3
CGRP is a chemical that causes the blood vessels around your brain to swell, while serotonin makes them shrink. If these chemicals are imbalanced, it can set the stage for pain and inflammation.
In addition, there are a few risk factors that can increase the chances of migraine, including:
- Genetics. According to the American Migraine Foundation, if one parent has migraine, their child has a 50% chance of developing it. If both parents have migraine, the risk shoots up to 75%.
- Women are three times more likely to suffer from migraine than men.5 Hormonal changes are believed to be the culprit.
- Certain health conditions are linked with migraine, including depression, anxiety, asthma, epilepsy, restless leg syndrome, heart disease, hypertension, and stroke.6
Migraine triggers
Migraine triggers vary from person to person. Common migraine triggers include:3
- Stress
- Hormonal changes
- Skipping meals
- Lack of sleep (or too much sleep)
- Changes in weather
- Strong scents like perfume or gasoline
- Bright lights
- Dehydration
- Certain foods including alcohol, chocolate, aged cheeses & foods containing food additives like aspartame, nitrates, and monosodium glutamate (MSG)
Other types of headaches
Now that you understand more about migraine, let’s cover some other headaches that may be mistaken for migraines.
Headaches generally fall into two categories: primary headaches and secondary headaches. Primary headaches, like migraines, are headaches without any clear cause. Secondary headaches, on the other hand, are due to an underlying health condition.7
There are over 150 different types of headaches. So clearly, we can’t cover them all in this article. But here are three other common types of headaches to watch out for:
Tension headaches
Tension headaches are the most common type of headache. Close to 80% of people get a tension headache now and then.8 They’re often described as a dull pressure or tightness spread around the head, much like wearing a tight hat or band. Like migraines, tension headaches are a type of primary headache. But unlike migraines, they usually occur on both sides of the head.
Stress, lack of sleep, and hunger are the most common causes of tension headaches.8 However, alcohol and menstruation can trigger them too. Unlike other types of headaches, physical activity doesn’t worsen their intensity.

Sinus headaches
Sinus headaches are secondary headaches that occur due to sinus infections. This can cause pressure to build in your sinus cavities, leading to pain in your cheekbones, forehead, or nose. If your headache comes with other symptoms like a runny nose, cough, fever, or facial pressure, it could be a sinus headache.
Sinus headaches are a sign your body is fighting off bacterial or viral infection. Once the infection is gone, the headache resolves. If the infection is due to bacteria, some people may need antibiotics. Unlike migraines, sinus headaches do not cause nausea or vomiting.
Sinus headaches are often most intense in the morning. Bending forward, lying down, or making sudden movements may worsen the pain.
Cluster headaches
As the name suggests, cluster headaches happen in “clusters.” Attacks occur several times a day for weeks or months, followed by periods of remission. They’re more likely to occur at night. A cluster headache usually lasts between 15 minutes and 3 hours.
Like migraines, cluster headaches cause severe pain on one side of the head. They start suddenly and create a sharp, burning, or piercing pain around or behind your eye. Other symptoms of cluster headaches include:
- Red or watery eyes
- Runny nose
- Droopy eyelid
- Flushing or sweating
- Restlessness
While women are more likely to get migraines, the opposite is true for cluster headaches. Men are three times more likely to suffer from cluster headaches than women. Smoking also increases the risk, as 88% of people who suffer from cluster headaches are smokers.
Like migraines, cluster headaches have many potential triggers, including:
- Alcohol
- Smoking
- Bright lights
- Hot weather
- Changes in altitude
- Exercise or exertion
- Foods containing nitrates like bacon or deli meats
- Stress
- Strong scents
Here’s a quick recap to help you compare the different types of headaches:
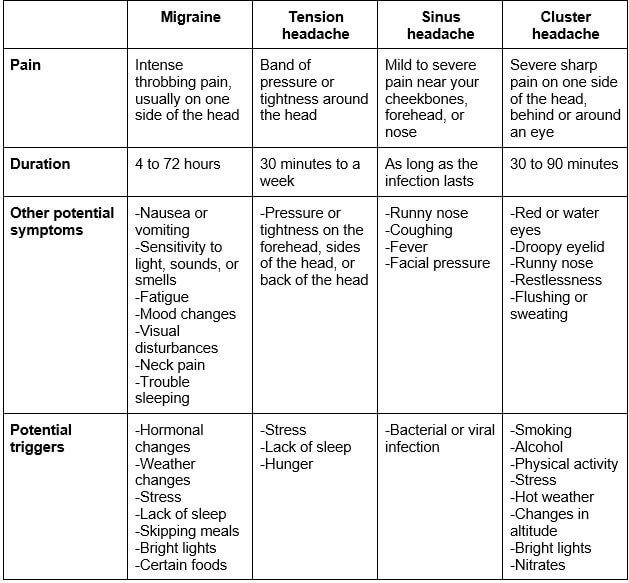
What’s the difference between migraines and headaches?
One key difference between migraines and other headaches is their intensity. Migraines are often so painful that they leave people unable to function. You may miss work, cancel plans, and struggle to keep up with simple day-to-day tasks.
Another major difference between migraines and other headaches is that migraines happen in phases with distinct symptoms. However, not all migraine sufferers experience each phase. Understanding the phases may help you recognize when you’re having a migraine.
The following are the four phases of a migraine attack:
Prodrome
Prodrome, also called the premonitory phase, is when your body sends signals that a migraine attack is coming.
Common prodrome symptoms include frequent yawning, mood changes, tiredness, and neck pain. This usually happens 24 to 48 hours before the headache kicks in.3
Aura
About 25% of migraineurs experience the second phase, known as ‘aura.’3 This phase is marked by sensory disturbances that affect a person’s vision, speech, or touch.
For some people, this may manifest as flashing lights, zigzags, blurred vision, or blind spots. Others may experience tingling or weakness in one limb or one side of the face. And while rare, some people may have trouble speaking. While aura can be intense, it’s usually over within an hour.
Headache
The third phase of migraine is when the headache finally hits. Migraine headaches involve throbbing or pulsing pain, usually on one side of the head. The pain can range from mild to downright debilitating. It can last anywhere between a few hours to a few days.
As the pain intensifies, other symptoms may be triggered including nausea, vomiting, and sensitivity to light, sound, and touch.
Postdrome
The last phase, postdrome, is sometimes called a “migraine hangover.” This is because its symptoms resemble what you might feel after a night of drinking. Common symptoms include exhaustion, dizziness, and trouble concentrating.
How to prevent migraines and headaches
Certain lifestyle shifts may prevent migraines and other headaches from occurring in the first place.
Here are some preventative tips to consider:
- Keep a migraine or headache journal. This can help you track patterns and identify any triggers contributing to head pain. Download your free migraine diary here.
- Reduce stress. Stress is a common trigger for migraines, tension headaches, and cluster headaches. So managing stress is crucial. To keep stress in check, set aside time each day for relaxation techniques like meditation, yoga, or slow, deep breathing.
- Exercise, but not too much. Research shows that regular exercise can help prevent migraine attacks from occurring.10 However, try not to overdo it. Strenuous exercise can trigger migraines and cluster headaches.
- Get enough sleep. Lack of sleep can trigger migraines and tension headaches. To keep headaches at bay, aim for 7 to 9 hours of sleep each night.
- Eat a healthy diet. Processed foods contain additives that can trigger migraines and tension headaches. Instead, opt for wholesome foods like fruits, vegetables, whole grains, nuts, seeds, and legumes.
- Get nutritional support. People with migraine are often running low on key nutrients like magnesium. Also, brain energy metabolism has been found to be disturbed in many people with migraine which can make the brain more sensitive to migraine triggers11– something high dose riboflavin can help correct. Nutritional supplementation can fill in the gaps an be very beneficial to migraineurs. Each daily dose of Migrelief gives you 360 mg of magnesium, along with 400 mg of riboflavin and 100 mg of Puracol feverfew to help maintain healthy cerebrovascular function , support brain cellular energy and healthy brain nerve transmission.

Keep a migraine diary
For more migraine prevention tips, check out this article.
Takeaways
Sometimes it’s hard to tell migraines apart from other types of headaches. But generally, migraines tend to be more debilitating and linger longer. If your headache lasts several days and comes with symptoms like nausea, vomiting, or visual disturbances, it could be a migraine. No matter your symptoms, if your headache doesn’t go away or keeps coming back, visit your healthcare provider.
Sources
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8904749/
- https://jamanetwork.com/journals/jama/fullarticle/2787727
- https://www.ncbi.nlm.nih.gov/books/NBK560787/
- https://americanmigrainefoundation.org/migraine-signs-symptoms/
- https://americanmigrainefoundation.org/resource-library/migraine-facts/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3008936/
- https://www.ncbi.nlm.nih.gov/books/NBK554510/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3444224/
- https://www.ncbi.nlm.nih.gov/books/NBK544241/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6134860/
- Riboflavin and migraine: the bridge over troubled mitochondria – PubMed (nih.gov)


