Sleep – or the lack thereof – is one of the most challenging aspects of fibromyalgia. On the one hand, research suggests that good quality sleep can improve fibromyalgia symptoms. But on the other hand, staying asleep throughout the night and feeling rested in the morning is extremely difficult when you have a pain condition.
What Is Fibromyalgia Anyway?
Before we delve into the specifics of how fibromyalgia affects sleep and talk about some strategies for managing sleep deprivation when you have a pain condition, it’s important to understand what fibromyalgia is.
Fibromyalgia is a medical syndrome characterized by widespread physical pain. This condition affects between 2 and 6 percent of the population, and women tend to be more likely to develop it than men. Even though fibromyalgia can occur to anyone of any age, it’s more common during early adulthood and middle age.
Not so long ago, medical professionals were still debating the existence of not just fibromyalgia but dozens of other pain conditions as well. The 16th century was the first time, as far as we know, that the medical community started thinking of pain as a condition instead of a symptom. In 1592, a French doctor named Guillaume de Baillou coined the term “rheumatism” to describe physical pain that didn’t stem from an injury. The name stuck for hundreds of years until physicians in the 19th century introduced more specific names.
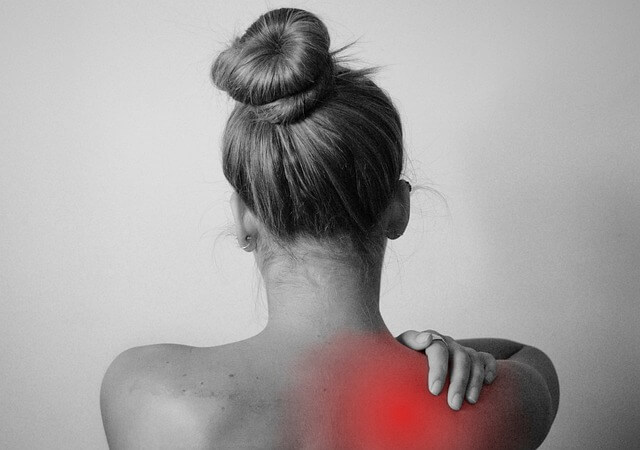
In the early 1820s, a group of doctors discovered that non-injury-related widespread pain was somehow connected to inflammation in certain nodes and nodules throughout the connective tissues of the body. These nodules later became the famous “tender points” that doctors used, until very recently, to diagnose fibromyalgia. The word “neuralgia” was created to describe the pain that irradiated from these tender points and traveled along the nervous system.
But the discovery and classification of fibromyalgia as a medical condition didn’t follow the same path of other diseases. Even though the criteria used to diagnose conditions varies widely, the information required to make an accurate medical diagnosis is usually a combination of the patient’s history and the results of one or more diagnostic or screening procedures. Diagnostic procedures can be lab or imaging tests, exploratory surgeries, and more.
In the case of fibromyalgia, however, experts are still trying to understand how and why it happens. The limited knowledge that we have of this condition means that physicians haven’t been able to develop a diagnostic test or procedure that can accurately identify the presence of this disease. In some cases, people are diagnosed with fibromyalgia when rheumatologists are unable to find another reason for their pain. Physicians also diagnose fibromyalgia by looking at the patient’s clinical history and by administering a questionnaire about symptoms.
The lack of diagnostic procedures and the fact that fibromyalgia shares many symptoms with other poorly understood conditions like depression, led many to believe that this was not a real condition. Contestants of fibromyalgia claimed that the chronic pain and other symptoms associated with this syndrome are a response to anxiety, depression, or other mental health disorders.
It wasn’t until 1976 that the name fibromyalgia and a more accurate description of the disease and its symptoms came about. Then, in 1990, the American College of Rheumatology established the official fibromyalgia diagnostic criteria, finally recognizing this debilitating syndrome as a real medical condition. In 2007, the FDA approved Lyrica, the first pharmaceutical drug to treat fibromyalgia.
Nowadays, we know that there are more than 100 different types of arthritis and several autoimmune conditions and syndromes – like fibromyalgia – that cause unexplained and sometimes debilitating widespread pain.
Fibromyalgia Symptoms
Even though widespread physical pain is the hallmark symptom of fibromyalgia, it is not the only one. People with this condition may also experience:
- Extreme sensitivity to touch
- Tenderness in or around the joints
- Joint stiffness
- Brain fog
- Irritable bowel syndrome (IBS)
- Migraines
- Tingling, burning or prickling sensations in hands or feet
- Anxiety
- Depression
And in the vast majority of cases, fibromyalgia also affects sleep.
Fibromyalgia and Sleep
The vast majority of fibromyalgia sufferers report poor sleep quality, restlessness, and fatigue. In fact, a 2011 research study published by the British Journal of Health Psychology with 104 women with fibromyalgia and 86 healthy controls showed that 98 percent of women with fibromyalgia had significant sleep problems in contrast with 38 percent of healthy controls.
For decades, healthcare professionals have theorized about the relationship between poor sleep and pain conditions. In the same study, researchers found poor sleep quality was also associated with increased pain, worst levels of self-efficacy and independence, anxiety, and depression. But it is not just that not sleeping enough can worsen the pain. Most fibromyalgia sufferers say that widespread pain is the number one reason why they cannot sleep through the night.
Fibromyalgia sufferers are also more likely to have other sleep disorders like obstructive sleep apnea (OSA). OSA happens when the muscles that line the airway relax too much, narrowing the throat and blocking air from reaching the lungs. One research study published by the American Journal of Medicine found OSA present in 44 percent of male fibromyalgia patients and in 22 percent of female patients.

But it’s not all bad news for people with fibromyalgia. Research suggests that lifestyle changes and some dietary supplements may help improve sleep quality and duration for people with pain disorders like fibromyalgia. These are some clinically proven drug-free tips and treatments for sleeping better when you have fibromyalgia.
What May Help to Improve Sleep
Vitamin D – a research study published in 2018 found that a vitamin D supplement can improve sleep quality of life of people with fibromyalgia and reduce morning stiffness. It is estimated that more than half of fibromyalgia patients have deficient or insufficient vitamin D levels, which is also associated with depression and anxiety.
Mindfulness Meditation – a 2007 analysis published by the American College of Rheumatology found that a type of mindfulness meditation called Mindfulness-Based Stress Reduction (MBSR) to be more effective than the standard treatment for depressive symptoms – including poor quality of sleep – among women with fibromyalgia.
Melatonin – melatonin is a naturally-occurring hormone made by the pineal gland that works with the circadian rhythm to signal the body when it is time to sleep. Preliminary research on the effects of melatonin on pain syndromes showed that people with fibromyalgia had lower night-time levels of fibromyalgia than other people. However, other studies have revealed mixed results.
Nonetheless, even when patients don’t have lower levels of melatonin, evidence suggests that melatonin supplements may help ease fibromyalgia and chronic fatigue symptoms, including depression and sleep deprivation.
To learn about a combination sleep supplement that contains melatonin and other ingredients proven beneficial for reestablishing health sleep patterns and promoting deep rejuvenating sleep, visit MySleepAllNight.com.
To download Akeso’s FREE Sleep-Ebook and Insomnia whitepaper CLICK HERE.


